How does the autism assessment go?
If your child possibly has autism (ASD) and goes in for an assessment, it is nice to know what you and your child can expect in advance. What steps will be taken? And how long will the process take? You can read about it on this page.
Your child goes in for the assessment to determine whether he/she has autism. It is then useful to know that the following points are important:
- A team of specialists conduct the assessment..
They have knowledge and experience in the field of diagnostics in young children. And especially in the field of autism in young children. - The team collects information from different people, such as:, zoals bij:
- parents/caregivers;
- leaders/teachers at daycare or school;
- other healthcare providers that are involved with your child;
- specialists from the organisation
- The team collects information in different ways. For example, by means of:
- questionnaires;
- interviews;
- reports of previous/other healthcare;
- observing your child in different situations (e.g. in play with you as a parent, during play with a professional, at school or at home).
- tests
The steps in the autism assessment
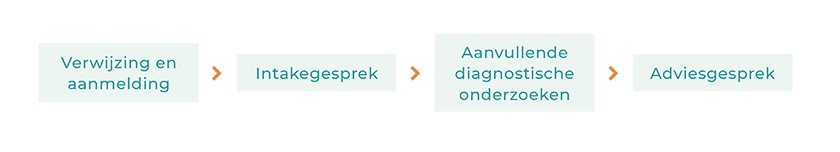
Exactly how the autism assessment proceeds and how long it takes varies per organisation. But it generally takes about six weeks. The following steps are usually followed:
1. Referral and registration
Your child has been referred to the specialised mental healthcare (GGZ). The organisation that will do the assessment checks to see whether the referral is justified. If it is, you will receive registration forms (in hard copy or digital). Usually you will also receive one or more questionnaires. In those, you will answer questions about the behaviour and development of your child, and questions about your family.
2. Intake interview
After you have registered your child, an intake interview will take place. You will meet with the child psychiatrist and/or psychologist/remedial educationalist. Your child is usually also present. In this interview, you will talk about various topics:
- the family situation
- previous healthcare
- the problems regarding the development and behaviour of your child
- your child’s strong suits
- your own request for help as parent(s)/caregiver(s)
After the intake interview, you will hear whether they will further assess your child, and if so how. These are additional diagnostic tests. During the intake interview, you also often hear who your care coordinator or contact person will be.
Tips for the intake interview with the GGZ organisation
(Source: Werkgroep ouders Lucertis, 2016) |
3. Further assessments
Examples of further assessments include:
- Further interviews with parents/caregivers;
- Observation of your child during play with you as parent(s)/caregiver(s);
- Observation of your child during play with a child psychiatrist or psychologist/remedial educationalist;
- Observation of your child in the home situation or at school;
- Tests aimed at identifying, for example:
- The level of mental development;
- The level of speech-language development;
- The development in the areas of attention, concentration and memory;
- Understanding of social situations or thoughts/feelings of others.
It may also be the case that another professional is observing as well. To get a complete picture of your child. For example:
- A paediatrician
- A paediatric neurologist
- A clinical geneticist
- A physiotherapist (he/she examines, for example, your child's motor skills and stimulus processing)
4. Consultation
First, the information from all the interviews and assessments is compiled. Then, a team of different specialists discusses this information. Each of them looks at the information from his/her own specialty.
A child and adolescent psychiatrist, a clinical psychologist or a gz-psychologist will ultimately assess whether your child has autism (diagnosis).
Sometimes, it is not entirely clear at the end of an autism assessment whether your child has autism. Perhaps it is another disorder. Your child is then given a preliminary diagnosis. We also call this a working diagnosis. Based on the working diagnosis, a plan is drawn up for the counselling/treatment of your child. While you are carrying out the plan, more will become clear about the problems. Sometimes, your child will then receive a different diagnosis.
In the consultation with you as parent(s)/caregiver(s), you will receive the diagnosis and get an explanation about it. You will also receive their advice on what possible counselling or treatment there is. There are essentially three possibilities:
- Your child and/or you do not need treatment/counselling (anymore). The course of treatment is completed.
- Your child and/or you do need treatment/counselling. A treatment/counselling plan is drawn up and this support is also provided within the same organisation, and/or;
- Your child and/or you are referred for (additional) counselling/treatment to another organisation.
Read more about the use of a (working) diagnosis of autism here..